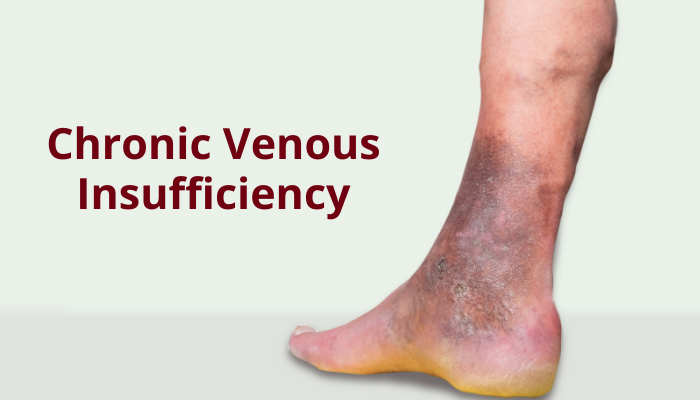
Chronic Venous Insufficiency (CVI) occurs when the venous wall or the valves in the veins of the legs are not working properly. This makes it difficult for the blood to return to the heart from the legs. CVI results in blood “pooling” or collecting in the leg veins and this is called “stasis”.
If you have CVI, you can experience one or more of the following chronic venous insufficiency symptoms in your legs: pain, swelling, cramps, skin changes, varicose veins, blood clots, and leg ulcers. While CVI is not a serious health threat, it can be disabling and painful. CVI is more common in women than in men. It is also more likely to occur in adults over the age of 50. In this article, we’ll talk at length about CVI…
Types of Chronic Venous Insufficiency (CVI)
CVI falls into three different categories, depending on the severity of the symptoms. These chronic venous insufficiency stages are:
- Stage 1: This stage presents with swelling and changes in skin pigmentation.
- Stage 2: This stage is characterized by swelling, changes in skin pigmentation and dermatitis.
- Stage 3: This stage is characterized by swelling, changes in skin pigmentation, varicose veins, and leg ulcers.
CVI can also cause chronic venous hypertension, a condition that is characterized by high blood pressure in the veins of the legs. Blood clots or other blockages in the veins can also lead to this condition.
If not treated, chronic venous hypertension can cause abnormalities in the capillaries within the legs, resulting in swelling, hyperpigmentation, and ulceration. In this condition, patches of skin become darker than usual.
Causes of Chronic Venous Insufficiency (CVI)
There are several causes of CVI. Some of them are:
- Obesity: If you are seriously overweight, you can develop CVI.
- Pregnancy: If you are pregnant, there is additional pressure on the leg veins, resulting in CVI.
- Family History: if your close family members have CVI, you are more likely to also develop it.
- Damaged legs: If you have damaged one or more legs due to injury, surgery, or one or more blood clots, you can develop CVI.
- High blood pressure in the legs: If you have high blood pressure in the leg veins due to sitting or standing for prolonged periods, this could result in CVI.
- Lack of exercise: A completely sedentary lifestyle can lead to CVI.
- A blood clot in a deep vein: A blood clot can occur in a calf or thigh vein, resulting in a condition called Deep Vein Thrombosis (DVT) and can also cause CVI.
- Phlebitis: This occurs due to swelling and inflammation of a vein close to the skin in the legs and can cause CVI.
Diagnosis of Chronic Venous Insufficiency (CVI)
Your physician will first conduct a physical exam to diagnose CVI. Your doctor will also review a person’s complete medical history and current health status before coming to a diagnosis of CVI. He may also conduct certain procedures to diagnose CVI. These include:
- Venogram: This uses X-ray technology to examine how blood flows through the veins. During this procedure, the contrast material is injected into a vein. Healthcare technicians and doctors also use venograms to locate blood clots and evaluate varicose veins.
- Duplex Ultrasound: This is a non-invasive test that examines the direction and speed of blood flow through the veins and arteries.
Other tests used to diagnose CVI include a CT scan, an MRI scan, and blood tests.
Prevention of Chronic Venous Insufficiency (CVI)
When it comes to CVI, prevention is definitely better than cure. Several of the risk factors associated with CVI are associated with a person’s lifestyle. By avoiding these risk factors, you may be able to prevent CVI. You can make certain lifestyle adjustments, such as:
- Getting regular exercise
- Avoiding wearing high heels
- Maintaining a healthy body weight
- Avoiding sitting or standing for prolonged periods of time
Treatment of Chronic Venous Insufficiency (CVI)
Despite preventive measures, if you develop CVI, it needs to be treated promptly. Chronic venous disease treatment includes:
- Improving the flow of blood in your leg veins: By keeping your legs raised, you can increase the blood flow and reduce swelling. You can also wear compression stockings and can take regular exercise.
- Medicines: Medicines that increase the blood flow through the vessels can be used along with compression therapy to treat CVI and prevent varicose veins and leg ulcers. Aspirin can also help leg ulcers heal. While medicines, such as diuretics, that draw excess fluid from the body through the kidneys are not often used, they may be used if other conditions such as kidney disease or heart failure are linked to the swelling.
- Endovenous Laser Treatment (EVLT): This is a procedure that uses laser heat to treat CVI and varicose veins. EVLT restores proper circulation in your legs. This procedure is minimally invasive, so you will not experience a lot of pain.
- Radiofrequency Ablation (RFA): This is a non-surgical, minimally invasive procedure that uses heat to treat CVI and varicose veins. This closes the veins and once the vein is closed, less blood pools in the legs. Also, overall blood flow is improved.
- Sclerotherapy: This can be used in severe cases of CVI. A chemical is injected into the affected veins. This chemical causes scarring in the veins so that they can no longer carry blood. The body then absorbs the scarred veins and blood returns to the heart through other veins.
- Surgery: This is done in severe cases and ligation is one such type of surgery that can be used. Blood no longer flows through the affected vein, which is tied off. If the vein or its valves are severely damaged, your vascular surgeon will remove the vein. This is known as vein stripping.
At the Flow Vascular Clinic, Dr. Abhilash Sandhyala is a skilled vascular surgeon and interventional radiologist. He is a varicose veins specialist and has treated several thousand cases of Chronic Venous Insufficiency (CVI) and Varicose Veins.
He knows exactly the kind of treatment you will need for your CVI and he is also an expert at EVLT. He will work with you individually to design a tailor-made treatment program just for you. So, if you have CVI or Varicose Veins, do not hesitate to consult with Dr. Abhilash Sandhyala, knowing for certain that you are in good hands!
For more information about chronic venous insufficiency (CVI), as well as the treatment for DVT, or other vascular conditions, contact Dr. Abhilash Sandhyala at (+91) 9989649498 or 9959033037, or at contact@drabhilash.com or visit our website.